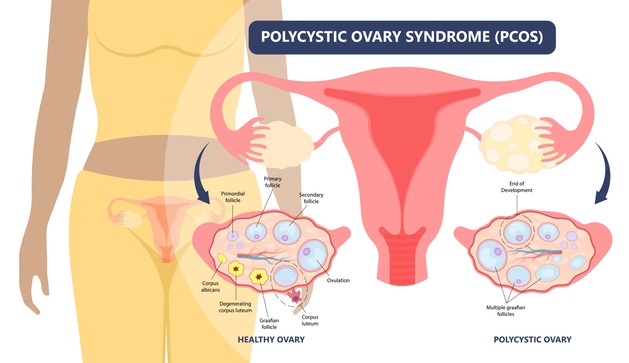
Yoga for PCOS: Polycystic ovarian syndrome, more commonly known as PCOS, is a widespread disorder affecting around 4% of the earth’s population. It manifests as a consequence of hormonal imbalances in the human body, which results in symptoms such as irregular and painful periods, weight gain, etc. With yoga for PCOS, the condition can be managed effectively.
In modern medicine, medical experts typically advocate a holistic approach to address the syndrome. And in the world of holistic healing, yoga for PCOS takes centre stage. Read on to find out which yoga poses work the best if you are battling with the condition of PCOS.

8 Most Effective Poses for PCOS and Boosting Fertility
People experiencing PCOS may have trouble conceiving a child because of irregular periods and high insulin resistance. However, this yoga for PCOS will help you regulate your cycle, control lipid levels in your blood, and manage insulin.
Remember, while performing all these yoga poses, keep your breathing even. Keep your shoulders relaxed and expand your chest for better airflow and posture.
Read Also: What is the PCOD Problem in Women And How Does it Affect Fertility?
1. Sun Salutation:
One of the best yoga poses, whether it is for weight loss, stress, or PCOS, is sun salutation. Traditionally performed at the break of dawn, these radiant postures can be practised at any hour, reaping the rewards of synchronised cycles and a reinvigorated physique.
However, you can perform them any time of the day and get benefits such as cycle regulation, weight loss, etc. This yoga pose is also recommended for controlling thyroid, which is another symptom of PCOS.
Read Also: What is Difference Between PCOS and PCOD?
2. Butterfly Pose:
This is the perfect yoga pose for improving fertility while relieving menstrual cycle pain. Easy to perform and maintain, the butterfly pose is also known as Baddha Konasaana. The pose requires you to sit with the heels of your feet touching or facing each other. The stretch this yoga for PCOS provides stimulates the digestive and reproductive systems.
3. Bridge Pose:
Bridge pose is a great way to relieve lower back pain. It also helps relieve stress and strengthen your back muscles, which will help you during pregnancy. The pose is easy to perform and can be done on your bed. Keep your feet aligned with your hips as you lie on your back. Inhale and lift your lower, mid, and upper back off the floor. Stay in the pose for a few minutes, then bring your pelvis back to the floor.
4. Cobra Pose:
Another yoga for PCOS that is widely recommended is the cobra pose. Also known as the Bhujangasan, the pose mainly strengthens your core, brings flexibility, and relieves stress. It soothes the digestive organs while increasing blood circulation in the pelvic region. The pose will also help regulate your menstrual flow and ease the pain.
One can also use this stress to improve their anxiety and stretch their upper body, including the neck and shoulders.
Read Also: Empowering Couples For Parenthood: Navigating Pregnancy With PCOS And PCOD
5. Boat Pose:
A great yoga pose that focuses on the abdominal muscles and pelvic region. Known as Naukasana in Sanskrit, the pose has been found to control the thyroid and improve fertility with regular practice. To do the pose, you must elevate your arms and legs off the floor to make a boat-like shape. Make sure that you inhale as you elevate them. Also, focus on your abdominal muscles to keep the pose steady.
6. Reclining Butterfly Pose:
This is a modification of the regular butterfly pose. However, it provides its own set of benefits. The pose stretches and helps open up the pelvic region. To do this yoga for PCOS, you must lie on your back and bring your heels against each other. Now, holding your feet together, bring them closer to your torso. Take this slow; you only need to stretch as much as possible. Hold the pose for a few minutes, and then straighten your legs.
7. Lotus Meditation:
Lotus Meditation, more commonly known as Padma Sadhna, is a series of yoga poses. It helps to relax your body, providing relief to your reproductive organs. The first pose of this series, known as the Padmasana, helps relieve pain experienced during the menstrual cycle. The series of yoga for PCOS followed under meditation are as follows:
- Pranayama
- Padmasana
- Makarasana
- Ardha Salabhasana
- Salabhasana
- Bhujangasana
- Viprit Salabhasana
- Dhanurasana
Each pose should be held for at least a minute to get its benefits. Also, after the complete series, you can do 10 minutes of meditation or 5 minutes of rest.
8. Standing Forward Bend:
Also known as Uttanasana, yoga for PCOS is beneficial as it allows better blood flow through the brain. It thus helps in relieving stress and easing anxiety. It also calms the nervous system. In essence, the pose, when held for a few minutes, will provide a therapeutic experience.
Read Also: Jackfruit During Pregnancy: Benefits, Risks, and Side Effects
The Bottom Line
Yoga poses are not only essential for physical health and fitness, but they also provide a way to a healthier mindset. The biggest issue with boosting fertility is having the right mindset and a positive outlook on the process. Yoga for PCOS can help you provide that mindset. When practised properly and regularly, any of these yoga poses will reduce the symptoms of PCOS and PCOD while also helping regulate your menstrual cycle.
Are you experiencing symptoms of PCOS? Whether you are looking to plan a pregnancy or a better quality of life, We can guide you through a research-backed treatment for PCOS.
Frequently Asked Questions About Yoga for PCOS:
Q: How often should I perform these poses in yoga?
Ans: You can perform the complete set of all the yoga poses listed here at least once daily. The yoga routine should be followed at least 4 to 5 days a week. However, make sure that you are not over-exerting yourself. Results from yoga are slow to appear.
Q: Is it safe to do these yoga poses whilst pregnant?
Ans: You will need to consult a professional, either your doctor or a certified yoga practitioner, to understand which yoga poses are safe to perform while pregnant. Also, different yoga poses are recommended for different stages of pregnancy.
Q: Is yoga a cure for PCOS?
Ans: Yoga for PCOS can help you manage and curb the symptoms of PCOS. There is no definite cure for PCOS, and you must watch your lifestyle, workout routine, and eating habits to notice a noticeable change.
Q: Is yoga beneficial for male fertility?
Ans: Yes, yoga is immensely beneficial for men and male fertility as well. Yoga has been proven to stimulate the glands, resulting in better growth of the testosterone hormone. It also helps in improving sperm health.
Q: How long before my fertility is affected by yoga practice?
Ans: Remembering yoga does not bring about a sudden change is essential. The results vary from person to person. You need to regularly practice the asanas, such as Bhujanasana, Lotus Meditation, Sun Salutation, etc., to get their benefits.
Read Also: What Is The Best Age To Get Pregnant With PCOS?
Read Also: PCOD Problem After Marriage: Reasons Behind Women’s Experience